NEONATAL MASTITIS
What is it?
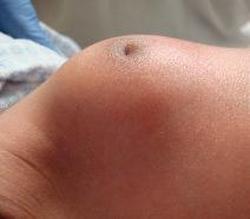
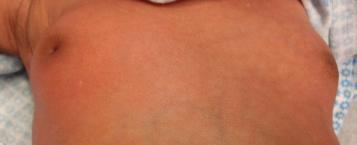
Neonatal mastitis typically occurs in full-term infants who are younger than two months. It is unilateral and local in nature. Characteristic clinical features include marked erythema, tenderness, and induration of the affected breast bud. Purulent nipple discharge and breast abscess may be present. The axillary lymph nodes may be enlarged and tender. Twenty-five percent of patients may also have fever (>101F (38.3C)). Between 50 and 100% of neonatal patients develop abscesses.
Systemic symptoms other than fever (e.g., irritability, decreased appetite, vomiting) are uncommon. Gastrointestinal symptoms may indicate Salmonella or other gram-negative enteric pathogens. Bacteremia is rare. Significant cerebrospinal (CSF) pleocytosis with sterile CSF culture may be seen in association with mastitis with or without systemic symptoms in patients infected with methicillin-resistant S. aureus. Cases of neonatal mastitis complicated by extensive cellulitis, necrotizing fasciitis, and osteomyelitis have been reported.
Diagnosis
In neonates, particular attention should be given to the presence of abscess formation, fever, and other systemic symptoms (e.g., poor appetite, lethargy) as these may indicate a serious systemic infection. If the lesion is fluctuant, purulent material from aspiration (with or without ultrasonographic guidance) or I&D also should be sent for gram stain and culture. If I&D are performed, it is important not to injure the underlying breast bud; appropriately trained personnel (e.g., a breast surgeon or pediatric gynecologist) should be consulted when this procedure is necessary. A CBC and blood culture should be obtained prior to antimicrobial therapy. If present, nipple drainage should be sent for gram stain and culture (aerobic and anaerobic). Urine and cerebrospinal fluid cultures should be obtained if these studies are clinically indicated (e.g., if the infant is febrile, ill appearing, younger than 28 days of age, or has leukocytosis).
Differential Diagnosis
It is important to distinguish mastitis from physiologic breast hypertrophy, which resolves spontaneously. In contrast to mastitis, in physiologic hypertrophy, the breast bud is neither red nor tender. The nipple discharge (if present) in physiologic hypertrophy is milky rather than purulent and does not contain polymorphonuclear white blood cells or bacteria on gram stain.
Treatment
No randomized controlled studies have evaluated antibiotic regimens for neonatal mastitis. Recommendations for treatment are based upon the causative pathogens and the response to therapy. Because of the potential for breast abscess, neonates should be treated with parenteral antibiotics guided by gram stain when available.
Neonatal mastitis be treated initially with parenteral antibiotics if the infant is febrile, ill appearing, has leukocytosis, or is younger than 28 days of age. An initial dose of parenteral antibiotics is also suggested in infants who are afebrile, well appearing, without leukocytosis, and older than 28 days of age, given the potential for progression to abscess in infants who are initially treated orally and the increasing prevalence of community-associated methicillin-resistant S. aureus. The empiric antibiotic choice should be guided by local susceptibility patterns and the gram stain, if one is available.
If gram-positive cocci are identified, empiric therapy should include coverage for S. aureus (e.g., clindamycin or vancomycin). If Gram-negative organisms are identified, empiric therapy should include an aminoglycoside (e.g., gentamicin, amikacin) or a third-generation cephalosporin (e.g., cefotaxime). If the gram stain is not available or if no organisms are seen, then therapy should include coverage for S. aureus and gram-negative enteric organisms. Therapy can be altered according to culture results once they are available.
Incision and drainage may be warranted if an abscess is present.
The duration of therapy depends upon the clinical response; a total of 7 to 14 days (parenteral/oral) is usually adequate if there are no complications.
Reference and further reading
http://www.uptodate.com/contents/search?search=mastitis+children&sp=0&searchType=0&source=USER_INPUT&searchControl=TOP_PULLDOWN&searchOffset=&autoComplete=true
What is it?
Neonatal mastitis typically occurs in full-term infants who are younger than two months. It is unilateral and local in nature. Characteristic clinical features include marked erythema, tenderness, and induration of the affected breast bud. Purulent nipple discharge and breast abscess may be present. The axillary lymph nodes may be enlarged and tender. Twenty-five percent of patients may also have fever (>101F (38.3C)). Between 50 and 100% of neonatal patients develop abscesses.
Systemic symptoms other than fever (e.g., irritability, decreased appetite, vomiting) are uncommon. Gastrointestinal symptoms may indicate Salmonella or other gram-negative enteric pathogens. Bacteremia is rare. Significant cerebrospinal (CSF) pleocytosis with sterile CSF culture may be seen in association with mastitis with or without systemic symptoms in patients infected with methicillin-resistant S. aureus. Cases of neonatal mastitis complicated by extensive cellulitis, necrotizing fasciitis, and osteomyelitis have been reported.
Diagnosis
In neonates, particular attention should be given to the presence of abscess formation, fever, and other systemic symptoms (e.g., poor appetite, lethargy) as these may indicate a serious systemic infection. If the lesion is fluctuant, purulent material from aspiration (with or without ultrasonographic guidance) or I&D also should be sent for gram stain and culture. If I&D are performed, it is important not to injure the underlying breast bud; appropriately trained personnel (e.g., a breast surgeon or pediatric gynecologist) should be consulted when this procedure is necessary. A CBC and blood culture should be obtained prior to antimicrobial therapy. If present, nipple drainage should be sent for gram stain and culture (aerobic and anaerobic). Urine and cerebrospinal fluid cultures should be obtained if these studies are clinically indicated (e.g., if the infant is febrile, ill appearing, younger than 28 days of age, or has leukocytosis).
Differential Diagnosis
It is important to distinguish mastitis from physiologic breast hypertrophy, which resolves spontaneously. In contrast to mastitis, in physiologic hypertrophy, the breast bud is neither red nor tender. The nipple discharge (if present) in physiologic hypertrophy is milky rather than purulent and does not contain polymorphonuclear white blood cells or bacteria on gram stain.
Treatment
No randomized controlled studies have evaluated antibiotic regimens for neonatal mastitis. Recommendations for treatment are based upon the causative pathogens and the response to therapy. Because of the potential for breast abscess, neonates should be treated with parenteral antibiotics guided by gram stain when available.
Neonatal mastitis be treated initially with parenteral antibiotics if the infant is febrile, ill appearing, has leukocytosis, or is younger than 28 days of age. An initial dose of parenteral antibiotics is also suggested in infants who are afebrile, well appearing, without leukocytosis, and older than 28 days of age, given the potential for progression to abscess in infants who are initially treated orally and the increasing prevalence of community-associated methicillin-resistant S. aureus. The empiric antibiotic choice should be guided by local susceptibility patterns and the gram stain, if one is available.
If gram-positive cocci are identified, empiric therapy should include coverage for S. aureus (e.g., clindamycin or vancomycin). If Gram-negative organisms are identified, empiric therapy should include an aminoglycoside (e.g., gentamicin, amikacin) or a third-generation cephalosporin (e.g., cefotaxime). If the gram stain is not available or if no organisms are seen, then therapy should include coverage for S. aureus and gram-negative enteric organisms. Therapy can be altered according to culture results once they are available.
Incision and drainage may be warranted if an abscess is present.
The duration of therapy depends upon the clinical response; a total of 7 to 14 days (parenteral/oral) is usually adequate if there are no complications.
Reference and further reading
http://www.uptodate.com/contents/search?search=mastitis+children&sp=0&searchType=0&source=USER_INPUT&searchControl=TOP_PULLDOWN&searchOffset=&autoComplete=true