MOLLUSCUM CONTAGIOSUM
What is it?
Molluscum contagiosum is a cutaneous infection caused by a large DNA poxvirus that affects both children and adults. Transmission of molluscum contagious has been reported by direct skin contact and has occurred in wrestlers, patients of a surgeon with a hand lesion, and children sharing baths, towels, gymnasium equipment, and benches. Autoinoculation also occurs as evidenced by linear arrays of lesions on infected individuals.
Differential diagnosis
Varicella
Basal cell carcinoma
Lichen planus
Dermatitis herpetiformis
Milia
Spitz nevus
Juvenile xanthogranuloma (Nevoxanthoendothelioma)
Warts, non-genital
Keratoacanthoma
Diagnosis
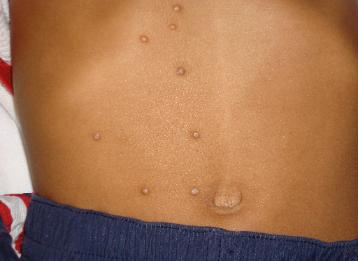
The diagnosis is often made clinically. Most patients are asymptomatic; some complain of pruritus, tenderness, and pain. Physical findings generally are limited to the skin, but cases have reported findings on the eyelids and conjunctiva. The lesions are firm, smooth, umbilicated papules, usually 2-6 mm in diameter (range 1-15 mm), may be present in groups or may be widely disseminated on the skin and mucosal surfaces. The lesions can be flesh-colored, white, translucent, or even yellow in color. In children, papules are located mainly on the trunk and extremities.
Treatment
Molluscum contagious generally is self-limited and heals after several months or years. Any one lesion is present for about 2 months; however, to prevent autoinoculation or transmission to close contacts, therapy may be beneficial. The common goal of the different treatment methods is the destruction of the lesions. The agents listed below have not been FDA approved for the treatment of molluscum.
Topical applications:
- Cantharidin - A single application that may need to be repeated once or twice every 3-4 weeks; gained popularity since being placed on a special FDA Bulk Substances List in 1997, allowing canthardin to be compounded and applied topically.
- Tretinoin cream (0.1%) or gel (0.025%) - Applied daily.
- Imiquimod cream 5%
- Trichloroacetic acid
- Cryotherapy with liquid nitrogen - One of the popular treatment modalities.
Systemic agents:
- Griseofulvin (Single case, anecdotal evidence)
- Methisazone (1methylisatin 2-thiosemicarbazone)
- Cimetidine
References:
www.uptodate.com
www.emedicine.com
What is it?
Molluscum contagiosum is a cutaneous infection caused by a large DNA poxvirus that affects both children and adults. Transmission of molluscum contagious has been reported by direct skin contact and has occurred in wrestlers, patients of a surgeon with a hand lesion, and children sharing baths, towels, gymnasium equipment, and benches. Autoinoculation also occurs as evidenced by linear arrays of lesions on infected individuals.
Differential diagnosis
Varicella
Basal cell carcinoma
Lichen planus
Dermatitis herpetiformis
Milia
Spitz nevus
Juvenile xanthogranuloma (Nevoxanthoendothelioma)
Warts, non-genital
Keratoacanthoma
Diagnosis
The diagnosis is often made clinically. Most patients are asymptomatic; some complain of pruritus, tenderness, and pain. Physical findings generally are limited to the skin, but cases have reported findings on the eyelids and conjunctiva. The lesions are firm, smooth, umbilicated papules, usually 2-6 mm in diameter (range 1-15 mm), may be present in groups or may be widely disseminated on the skin and mucosal surfaces. The lesions can be flesh-colored, white, translucent, or even yellow in color. In children, papules are located mainly on the trunk and extremities.
Treatment
Molluscum contagious generally is self-limited and heals after several months or years. Any one lesion is present for about 2 months; however, to prevent autoinoculation or transmission to close contacts, therapy may be beneficial. The common goal of the different treatment methods is the destruction of the lesions. The agents listed below have not been FDA approved for the treatment of molluscum.
Topical applications:
- Cantharidin - A single application that may need to be repeated once or twice every 3-4 weeks; gained popularity since being placed on a special FDA Bulk Substances List in 1997, allowing canthardin to be compounded and applied topically.
- Tretinoin cream (0.1%) or gel (0.025%) - Applied daily.
- Imiquimod cream 5%
- Trichloroacetic acid
- Cryotherapy with liquid nitrogen - One of the popular treatment modalities.
Systemic agents:
- Griseofulvin (Single case, anecdotal evidence)
- Methisazone (1methylisatin 2-thiosemicarbazone)
- Cimetidine
References:
www.uptodate.com
www.emedicine.com